The Science of Spinal Health: Why Movement Matters More Than You Think
The spine is more than a central pillar that keeps us upright. It is a dynamic, living system engineered to respond to movement, load, and stretch. In modern life, we often treat the spine as something to protect with rigid routines, couch cushions, and careful avoidance of discomfort. Yet the science is clear: movement is not a luxury for spinal health-it is a foundation. From the micro-scale of disc nutrition to the macro-scale of posture and daily activity, movement matters. This article dives into the anatomy of the spine, how movement feeds its tissues, the myths that mislead us, and practical ways to design a routine that supports long-term spinal health. If you've ever wondered why your back hurts with inactivity and improves with movement, you're in the right place.
The spine in plain terms: structure, function, and why it's uniquely sensitive to movement
Think of the spine as a column made up of building blocks (vertebrae), cushions between them (intervertebral discs), joints at each segment (facet joints), ligaments, muscles, and a highway (the spinal cord and nerve roots) that carries information to and from the brain. Each component plays a distinct role, but they work as an integrated system. The bones provide structural support, the discs dampen impact and allow for motion, the joints enable bending and rotation, and the muscles stabilize and power movement. Ligaments help limit excessive motion and protect sensitive neural tissue. When the system moves well, you feel flexible, strong, and resilient. When it does not, even small tasks can become painful or exhausting.
Intervertebral discs are particularly fascinating and often misunderstood. Each disc has a gelatinous center called the nucleus pulposus surrounded by a tougher outer ring called the annulus fibrosus. The discs are largely avascular, meaning they don't have a direct blood supply. Instead, nutrients reach the disc through diffusion from surrounding tissues, especially via the endplates of adjacent vertebrae. This nutrient exchange is enhanced by movement and loading that alternates pressure across the disc, effectively "pumping" fluids in and out. In simple terms: movement helps the disc stay nourished and healthy. When we stay immobile for long periods, the diffusion-driven nourishment can lag, and over time the disc may become stiffer and less effective at distributing loads. This isn't a doom-lent narrative, but it helps explain why sedentary habits correlate with back discomfort for many people.
Muscles-particularly those of the core, back, hips, and pelvis-are the engines that organize and control spinal movement. They don't just hold you up; they coordinate with your breathing, your posture, and your daily activities. Strong, well-timed muscle activation supports the spine during lifting, bending, and reaching. It also modulates how forces travel through the vertebral column, which can influence injury risk and pain levels. In other words, movement is not optional for the musculature that protects and powers the spine-it's essential.
How movement nourishes spinal tissues: the science behind "motion is lotion" for the spine
Two ideas help illuminate why movement is so crucial for spinal health: diffusion-based nourishment of avascular tissues (notably the discs), and mechanotransduction-the way tissues sense and respond to mechanical stimuli. Both concepts rest on the simple truth that load and movement drive biological processes in the spine.
First, the discs rely on diffusion for nutrients and the removal of waste products. Because the nucleus pulposus has little direct blood supply, it depends on nearby tissues and the endplates to exchange fluids and solutes. When you sit immobile for long periods, the rate of this exchange can slow, and the disc's internal environment may shift toward less favorable conditions. On the flip side, regular, varied movement facilitates gentle loading and unloading cycles that promote diffusion and exchange. The result is better hydration, maintenance of disc height, and improved resilience against everyday stresses.
Second, mechanotransduction describes how cells within the spine respond to mechanical forces. When you move, your cartilage, ligaments, and bone respond by remodeling their internal architecture in directions that strengthen the tissue against anticipated forces. This isn't about becoming fibrotic or stiff; it's about tuning tissues to handle the loads of daily life-lifting groceries, tying shoelaces, playing with kids, or walking up stairs. Consistent, progressive loading fosters healthier matrix production and protects against degeneration that can come with disuse. The take-home message: movement provides the signals that keep spinal tissues adaptable and robust rather than brittle or deconditioned.
Movement also helps manage neural factors related to pain. When you are inactive, the nervous system can become more sensitive, amplifying even minor discomfort into a painful experience. Gentle, controlled movement, exposure to varied motions, and gradual progression can reduce this amplification through a combination of improved tissue condition and altered central nervous system processing. In short, movement doesn't just physically load the spine; it also recalibrates the way your brain perceives spine-related sensations.
Common myths about spinal health and movement-and what the science actually says
Myth 1: If my back hurts, I should rest completely until pain goes away. Reality: While rest can be useful for a short period after an acute flare, prolonged inactivity tends to reduce tissue tolerance and can worsen pain sensitivity. Gradual, progressively loaded movement tends to improve function and reduces fear-avoidance behaviors, which often perpetuate pain cycles. The optimal approach is typically to stay gently active within pain limits and to resume meaningful movement as soon as possible.
Myth 2: Bending or twisting the spine is dangerous and should be avoided. Reality: The spine is designed to move through bending, flexion, extension, lateral bending, and rotation. Problems arise when movements are performed with poor form, with high loads, or when pain signals are ignored. Controlled, well-taired mobility and bending patterns-within a person's anatomical limits-are a normal and healthy part of spine function.
Myth 3: You need intense, high-load workouts to protect the spine. Reality: For most people, especially those without preexisting conditions, a balanced mix of moderate aerobic activity, mobility work, and a progressive resistance routine yields better spine health than occasional maximal efforts. More important than extreme intensity is consistency, gradual progression, and attention to technique.
Myth 4: Pain equals damage. Reality: Pain is a complex signal that reflects tissue state, nervous system sensitivity, and psychosocial factors as well as actual tissue injury. Pain does not always map cleanly onto tissue damage. A thoughtful movement plan that respects pain thresholds and uses gradual, graded exposure often reduces pain over time even when imaging stays unchanged.
Movement modalities that support a healthy spine: practical options you can adopt
Below are movement strategies that align with how the spine is built and how it responds to use. These are not exotic routines; they are practical ways to weave movement into daily life in a safe, sustainable manner.
Walking and general aerobic activity provide the simplest, most accessible foundation. Regular brisk walks, cycling, swimming, or dancing improve blood flow, circulation of nutrients to spinal tissues, and overall fitness. Aim for at least 150 minutes per week of moderate-intensity aerobic activity, broken into manageable sessions. If you're new to exercise, start with 10-15 minutes and gradually increase. Over time, you will notice improvements in endurance, mood, and how your back feels during daily tasks.
Core stability and trunk control are central to spinal health. Core training doesn't mean endless sit-ups. It means learning to brace and stabilize the trunk while performing functional movements. Start with gentle, coordinated activation of the deep abdominal and back muscles during everyday activities, then progress to controlled exercises that involve the pelvis and ribcage moving in harmony. The goal is a stable, well-coordinated core that helps transfer forces between the lower and upper body without overloading the spine.
Mobility and flexibility work should emphasize the spine's natural ranges and the joints that influence spinal mechanics, such as hips, thoracic spine, and shoulders. Gentle mobility routines-like seated or supported cat-camel sequences, thoracic rotations, hip hinges, and ankle-to-knee stretches-can reduce stiffness and improve movement quality. Move with breath, targeting smooth, pain-free ranges rather than forcing extremes. Consistency beats intensity here: short daily sessions beat infrequent, long ones.
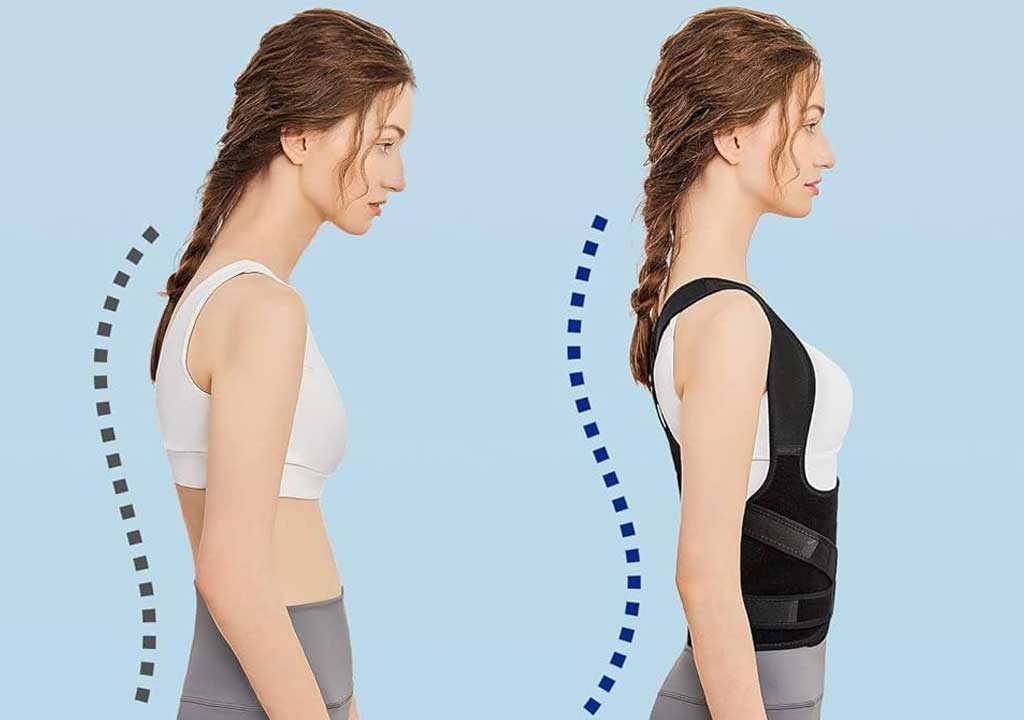
Posture and ergonomic considerations matter, particularly for people who sit at desks for extended periods. Neutral spine alignment with ergonomically arranged screens, chairs, and keyboards reduces unnecessary loading on the lower back. Small habits-standing up every 30-60 minutes, taking a short walk, and performing light mobility during breaks-compound over weeks and months to reduce cumulative strain. If you work at a computer, consider a sit-stand workstation and a chair that supports the natural curves of the spine.
Strength training is a powerful ally for spinal health when approached sensibly. Focus on balanced programming that targets major muscle groups, including the glutes, hamstrings, back extensors, and core muscles. Prioritize technique over the amount of weight and progress gradually to avoid overload on the spine. Compound movements such as squats, deadlifts (with proper form and lighter loads as needed), push-pull patterns, and hip hinges support spine health by improving load distribution across the entire chain. If you're new to lifting or have a history of injuries, seek instruction from a qualified professional to tailor a plan to your needs.
A holistic routine also considers breath and pelvic floor health, because breathing mechanics influence core stabilization. Diaphragmatic breathing can support intra-abdominal pressure regulation and reduce undue strain on the spine during exertion. Gentle pelvic floor work may also contribute to spinal stability, particularly for individuals with specific postural or functional concerns.
Putting it into practice: a practical, science-backed routine you can start today
Here's a simple, scalable plan that emphasizes consistency, safety, and gradual progression. It's designed to be doable in most homes or small gyms and to integrate seamlessly with daily life. Adjust the duration and intensity to your current fitness level and any medical guidance you've received. If pain persists or worsens, pause and consult a healthcare professional.
Warm-up (5 minutes): Gentle movement to prime the spine and surrounding tissues. Examples: slow marching in place, ankle circles, gentle shoulder circles, light hip circles, and diaphragmatic breathing with relaxed shoulders. The goal is to raise temperature and prepare the nervous system for movement without provoking pain.
Mobility block (5-8 minutes): Focus on thoracic spine and hips to improve load transfer and reduce compensations. Examples: seated cat-camel with paced breathing (8-12 reps), thoracic rotations (6-8 reps per side), hip hinges from a chair with a small hinge range (8-12 reps), and ankle-to-knee mobility for the hips to ensure pelvic stability during movement. Move through each exercise with control and ease, never forcing ranges.
Stability and strength block (8-12 minutes): Build a foundation of core and back stability with low to moderate loads. Sample sequence (perform as a circuit, 2-3 rounds):
- Bird-dog: 8-12 reps per side, smooth and controlled.
- Glute bridge: 12-15 reps, focusing on pelvis alignment and gradual hamstring engagement.
- Side plank (modified if necessary): 15-30 seconds per side, with hips stacked and a stable trunk.
- Row variations (bodyweight or light dumbbell): 8-12 reps, keeping shoulders down and back, avoiding excessive spinal extension.
- Hip hinge to chair/bench: 10-12 reps, emphasizing hinge from the hips rather than rounding the spine.
Adjust reps and sets to your tolerance and progress gradually over weeks.
Conditioning and cooldown (5-10 minutes): Finish with low-impact cardio to promote circulation and a gentle cooldown that emphasizes breath and stretch. A brisk 10-minute walk, light cycling, or easy swimming can be excellent options. End with a few minutes of gentle spinal stretches or mobility work at a comfortable range. Finish with a slow, diaphragmatic breath cycle to promote relaxation and reduce residual muscle tension.
Weekly progression ideas:
- Increase one element at a time: add 5-10% more weight or one extra repetition every couple of weeks, or extend a hold by a small amount.
- Swap in an additional mobility exercise every week to keep the routine fresh and address new stiffness areas.
- Mix in one longer day of light activity (a longer walk or easy hike) to reinforce the habit.
Consistency is more important than intensity. The spine benefits from repeated, moderate loading over weeks and months, not sporadic, maximal efforts.
Why movement helps more than you might expect: chronic pain, function, and aging
Movement does more than support the mechanical aspects of the spine. It interacts with the brain, nerves, and even hormones in ways that influence how we experience pain and how our bodies age. People who stay more physically active tend to have better spinal function, less disability from back pain, and improved quality of life as they age. Movement can reduce the likelihood of deconditioning-the gradual loss of muscle, bone, and connective tissue strength-and can help preserve the disc's nutrition by fostering healthy exchange of fluids and metabolites. It also helps with sleep, mood, and energy-factors that feed back into how we perceive and tolerate discomfort.
It's also worth highlighting the social and psychological dimensions. The spine does not exist in a vacuum; our daily routines, stress levels, sleep quality, and social support all influence spinal health. Movement provides a constructive, non-punitive way to engage with your body and can empower you to participate more fully in life's activities. When we treat movement as medicine-not as a dreaded chore-sustained habits become natural, not negotiable.
Addressing common concerns for different life stages
For office workers: The key is to interrupt prolonged sitting with micro-mulses of movement and posture variation. Short, regular breaks; a stand-up desk; a few mobility moves during breaks-these small actions add up to a meaningful improvement in spinal comfort over time.
For parents and caregivers: Lifting children and carrying loads happens in unpredictable patterns. Training around proper bending mechanics, hip hinge technique, and core control reduces strain and protects the spine during daily duties. A weekly routine that reinforces safe lifting, combined with mobility and conditioning, builds resilience.
For older adults: Movement remains essential, but safety and gradual progression are paramount. Emphasize balance, stability, and gentle mobility to prevent falls and maintain independence. Load-bearing activities should be introduced carefully, with attention to joint comfort and any preexisting conditions. Always consult a clinician before starting a new program if you have a history of osteoporosis, osteoporosis-related fractures, or spinal surgery.
Putting it all together: the bigger picture of spinal health
Movement is a bridge between the biology of spinal tissues and the lived experience of daily life. A healthy spine isn't a rigid spine; it's a well-tuned system that can adapt to a wide range of activities. The science supports a simple truth: regular, varied movement that respects your body's limits improves tissue health, reduces pain, and enhances function. It helps discs stay nourished, joints stay lubricated, muscles stay strong, and nerves stay resilient. It also supports mental well-being and sleep, which, in turn, reinforces the body's capacity to move well.
In practice, that means designing a movement plan that you can stick with-one that includes aerobic work, mobility, core stability, and strength-while listening to your body. If something hurts in a way that feels sharp, escalating, or unusual, pause and seek professional guidance. Pain is a signal that deserves attention, not a cue to push through blindly. The goal is sustainable movement over time: tiny, consistent steps that accumulate into lasting health.
Closing thoughts: your spine's future is written by today's choices
Spinal health is not destiny, but it is time-sensitive. The tissues that form the spine respond to how we treat them. Movement is a powerful tool that helps nourish discs, stabilize the spine, and protect neural function. It reduces fear around pain, improves function, and enhances overall well-being. The science is clear: stay as active as your body allows, mix up movement to address all the joints and tissues involved, and progress gradually with attention to form and safety. A small daily commitment to movement can transform not only how your back feels but how you experience life-from lifting a child to climbing stairs, from a morning walk to an evening stretch. Your spine's health story isn't written in a single day; it's written in the habits you choose each day. And the best habit of all is to move, again and again, with curiosity, care, and consistency.
Final note: a quick checklist to keep you on track
Use this mental checklist to guide your daily and weekly routines:
- Do you move with variety: aerobic activity, mobility, and strength work?
- Are you progressing gradually, with good form, and without pain?
- Do you take breaks from prolonged sitting or static postures?
- Are you sleeping well and managing stress, both of which influence spinal health?
If the answer is yes to these questions, you're likely on a solid trajectory toward a healthier spine. If not, adjust one variable at a time and give your body time to adapt. Your future self will thank you.
Conclusion
The science behind spinal health is both intuitive and nuanced. Movement serves as the lifeblood of the spinal system, delivering nutrients to avascular tissues, guiding tissue remodeling, and training the nervous system to interpret and respond to signals efficiently. Rather than fearing movement or chasing extreme solutions, the most reliable approach is consistent, measured movement that respects individual limits and goals. From simple daily walks to a balanced routine of mobility and strength training, small, deliberate steps accumulate into meaningful improvements in posture, pain, and function. The spine is built to move, and with science-backed movement strategies, you can give it the care it deserves-today, tomorrow, and for many years to come.
Thank you for reading. If you'd like, I can tailor a personalized, step-by-step progression based on your current activity level, any back pain history, and your daily schedule. The best plan is one you can follow consistently, and I'm here to help you design it.